
- NCDs (Non-communicable Diseases) often known as the chronic disease, are the set of the disease that cannot be transferred from one person to another. NCDs do not occur from acute infection rather it results from the lifestyle and other multiple causes.
- NCDs does not occur spontaneously as they are resulted by the sum of individual’s behavior and activities till the date of occurrence of disease.
- Four main types of NCDs are:
- cardiovascular diseases (like heart attacks and stroke)
- cancers
- chronic respiratory diseases (like chronic obstructive pulmonary disease and asthma) and
- diabetes
- Furthermore, it also includes mental illness, musculoskeletal disease, injuries etc.
Table of Contents
Disease burden due to NCDs:
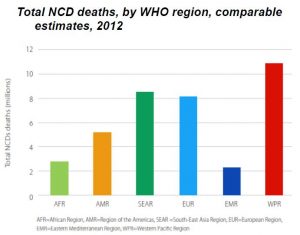
- NCDs are the cause for the death of 41 million people (annually) around the globe, which is 71% of the total deaths.
- Among the NCDs, cardiovascular diseases (15 million) is responsible for maximum death followed by cancers (9 million), respiratory diseases (3.9 million), and diabetes (1.6 million). These four diseases account for 80% of all premature NCD deaths [2018 WHO].
- Among the top 10 causes of death in the year 2016, 8 out of 10 diseases (conditions) are NCDs. Ischemic heart disease ranks the first position followed by stroke, pulmonary disease and others.
- NCDs are not only associated with death but with disability as well.
Are NCDs an important issue?
- The global burden of the NCDs is increasing yearly. Disease burden shifted from the communicable disease to NCDs. Similar increasing trend of NCDs could lead to pandemic
- NCDs causes premature death, disability and has huge economic burden as well.
- The treatment of NCDs would lead to catastrophic health expenditure.
- NCDs mostly effects the low and middle income countries thereby increasing the burden tenfold times.
- NCDs not only effect health of single individual but also acts as the major hindrance for development, progress and is highly associated with poverty.
Risk factors for NCDs:
Risk factors of NCDs can be identified as modifiable and metabolic risk factors. They are
- Modifiable risk factors: These are the risk factors which can be modifiable/changed for increasing or decreasing the risk of NCDs.
– Smoking
– Alcohol consumption
– Physical inactivity
– Unhealthy diet

- Metabolic risk factors: It includes four key metabolic changes in the body that might increase the risk of NCDs.
– Hypertension/high blood pressure
– Hyperglycemia (high blood glucose)
– Hyperlipidemia (high level of fat in the blood)
– Overweight/obesity
Causation Pathway for chronic NCDs:
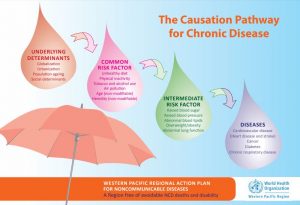
Contributory factors to NCDs:
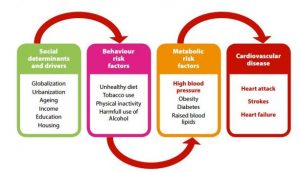
Source: WHO, 2014
Different interventions to address NCDs and its risk:
1. Population wide interventions:
- Reduce tobacco use
- Promote physical activity
- Reduce harmful use of alcohol
- Promote healthy diet
2. WHO best buys interventions:
WHO has identified the interventions for NCDs, also known as “best buys”. These interventions are very cost effective, easily adaptable, suitable and effective. They are:
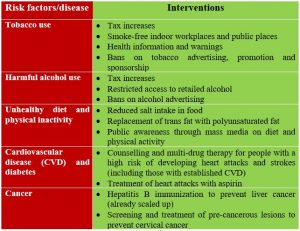
Source: WHO, 2011
3. Life style interventions:
Some major life style interventions could be:
a) Education:
- Education is the key to every intervention.
- Health education regarding NCDs acts as the motivational factor and also enables person to have control over own health.
- Creates awareness
b) Healthy diet:
- Diet is also the determining factor for the NCDs
- Encouragement and priority to the healthy foods
- Avoid packed, junk, canned and take away foods
- Inclusion of variety of vegetables and fruits in the diet
- Low intake of food containing trans fatty acids
c) Discourage smoking and alcoholism:
- Tobacco, its products and alcohol are to be avoided
- This can be done through government level by casting more tax on such products.
- Banning the advertisement of their use.
d) Healthy living:
- Giving up the sedentary lifestyle
- Exercise and increase the physical activity
- Walk when you can
Note: NCDs demands attention from individual, governmental and global level. Along with lifestyle interventions, medical interventions, disease specific interventions, etc., are necessary to prevent NCDS.
Challenges to address the NCDs:
a) Insufficient resources to meet up with the global outbreak
- With the incidence and burden of NCDs increasing each year, resources are insufficient to meet up.
- Both financial and human resource are not adequate.
- Inequitable distribution of health workers further adds up the problem.
b) Lack of commitment
- Lack of Commitment is the serious challenge for addressing the NCDs
- Neither the government nor public are committed about the interventions to address NCDs.
- Health is usually less prioritized and NCDs even lesser, especially in developing countries
- Government barely accept that the risk factors of NCDs are more related to socio-economic status than health factors.
- Unlike communicable disease, NCDS requires Behavior Change Communication (BCC) approach. People are less committed to adopt the healthy lifestyle
- High level of illiteracy too affects and acts as a barrier.
- Multi-sector involvement and global partnership is necessary to solve the problem of NCDs. Such partnership and commitments are hard to maintain practically.
c) Double burden of disease
- We are currently facing the double burden of disease
- Disease like diarrhea still claims the life of thousands of the people.
- With CDs still killing people NCDs are given less priority
- NCDs degrades the health as well as economic status further deepening the burden
d) Lack of Researches
- Researches regarding NCDs is not enough
- Region specific studies are lacking
- Research culture and its adaptation to policy is poor in many countries
- Evidence based interventions are lacking
References and for more information:
http://www.who.int/gho/mortality_burden_disease/causes_death/top_10/en/
https://www.gacd.org/research/what-are-ncds
http://www.who.int/nmh/publications/best_buys_summary.pdf
https://www.ncbi.nlm.nih.gov/books/NBK10246/
https://www.gacd.org/research/what-are-ncds/chronic-diseases-fact-sheet
http://www.wfpha.org/tl_files/images/Newsletter%202012/May%202012/NCDP%20Program%20Overview.pdf
http://www.who.int/news-room/fact-sheets/detail/noncommunicable-diseases
http://www.who.int/bulletin/volumes/94/3/15-156869/en/
https://ncdalliance.org/news-events/blog/reflections-on-the-2015-global-burden-of-disease-report
https://academic.oup.com/eurheartj/article/36/31/2097/2398206
http://www.emro.who.int/images/stories/ncd/documents/Tehran_meeting-_final_report_2.pdf
http://www.who.int/nmh/events/global_forum_ncd/forum_report.pdf?ua=1